There were 4 separate readings: 2 using only xR and 2 using only CT scans. Pictorial representations of the various fracture patterns were available to use by surgeons during their respective classification sessions. Regarding CT assessment, each surgeon was provided access to all DICOM files so that the surgeons could visualize 2-dimensional images as well as 3-dimensional renderings at their discretion.īefore initiating the study, the 3 surgeons met for a 1-hour training session to discuss all details of the pattern-based Mayo-FJD classification. XR Were cleared of patient identifying data by an independent research assistant and provided to each of the surgeons. 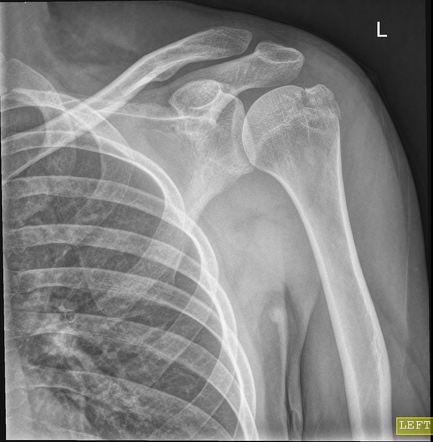
To be included in this study, anteroposterior and axillary xR and a CT scan had to be available for assessment. Three trained shoulder surgeons blindly and independently assessed the xR and CT obtained during the evaluation of 103 consecutive PHFs treated at a Level I trauma center between June 2019 and June 2020. As such, the purpose of this study was to evaluate the intraobserver and interobserver agreement of the pattern-based Mayo-FJD classification system of proximal humerus fractures on both using plain radiographs (xR) and computed tomography (CT). This pattern-based Mayo-FJD classification system includes 7 common patterns described in the material and methods section.Īlthough the authors have used this classification system in their practice for years, a formal attempt to assess its intraobserver and interobserver agreement has not been completed to date. 2, 8 A new classification scheme based on pattern recognition was developed to first identify the fracture pattern and only then apply displacement criteria to each pattern, thus separating fracture pattern from fracture displacement. 19ĭuring a research project between Mayo Clinic and Fundación Jiménez Díaz (FJD), 2 of the authors of this study realized that the majority of proximal humerus fracture (PHF) followed specific patterns best identified in 3-dimensional renderings of computed tomography. When using a morphologic classification system, the reproducibility is improved. 15 In contrast with classification systems for fractures of other bones, most proximal humerus fracture classifications mix fracture displacement and fracture parts or segments when defining the various categories. 3, 7, 11, 14, 20, 22 Other classification systems developed later, such as the Arbeitsgemeinschaft für Osteosynthesefragen - Association for the Study of Internal Fixation, Eldelson's, or Hertel's, have not demonstrated adequate reproducibility 10, 14, 22 or prognostic value 1, 5, 6 although recent modifications of the Arbeitsgemeinschaft für Osteosynthesefragen - Association for the Study of Internal Fixation published in 2018 improved its performance. 21 Similar results, with poor-to-fair reliability, have been found by other authors when assessing the Neer classification. Siebenrock and Gerber reported mean kappa coefficients for interobserver and intraobserver reliability of 0.40 and 0.60, respectively. Multiple studies have failed to demonstrate adequate levels of agreement or a definitive prognostic value of the Neer classification. As displacement is a continuum, there will always be some borderline lesions.” 17 Furthermore, Neer wrote that his classification scheme was “not intended to dictate treatment. 4 Neer disclosed in a 2002 review of his own classification that “the limits of 1.0-cm displacement or 45° angulation were arbitrarily set” at the request of Brown, the editor of Neer's original article. 16, 17 It was developed in the 1970s based on radiographic analysis and the concept of fracture segments first described by Codman. 
Until now, the classification proposed by Neer remains the most widely accepted system. Development of a useful classification system for proximal humerus fractures has remained elusive.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
